This guest post was written by Payton Jones (payton_jones@g.harvard.edu) and Haley Elliott (haleyelliott@college.harvard.edu), and is based on a recent letter in which they highlight the importance of non-symptom variables in psychological networks. Payton is a graduate student at Harvard University in the Richard J. McNally lab. His research focuses on the etiology of mental disorders and statistical methods. Haley is an undergraduate research assistant, also in the McNally lab at Harvard.
If you are reading this, it is likely that you have heard of the network approach to mental disorders. Since the dawn of medicine, scientists have tried to isolate disorders which give rise to symptoms. Just a few years ago, the network approach to mental disorders flipped this view on its head by asserting that some problems may in fact represent interacting symptoms which give rise to disorders.
This view has been revolutionary, sparking the advent of important new research. However, after several years following the network view, the initial tenets may need to be expanded.
In a recent review of the network approach, Denny Borsboom elucidated four key principles of the initial network view. Principle 2, in particular, states that mental disorders are best represented by networks emerging from interactions among “nodes”, which correspond to symptoms from diagnostic manuals.
It seems evident to clinicians and researchers alike that symptoms do indeed interact with one another, and certainly play a role in the emergence of mental disorders; but can we really blame them for everything?
Where do symptoms in diagnostic manuals come from?
Part of the problem with using symptoms from diagnostic manuals comes from the imperfect history of psychopathology research. Symptoms from the DSM or other manuals are not God-given – they have been carefully chosen by past researchers, often using consensus as a final criterion. Unfortunately, they were not picked with the network perspective in mind. Instead:
1) Symptoms are designed to differentiate between disorders.
Past researchers often gave precedence to “hallmark” symptoms that were unique to a specific problem, and easily differentiable from other problems (such as anhedonia in depression). This means that diagnostic manuals often ignore symptoms that are shared among many disorders, such as concentration problems and sad mood. Ironically, these “transdiagnostic” features seem to be some of the most important nodes in at least some recent network analyses.
2) Symptoms are distressing
Symptoms are generally only identified if a patient or their family identifies them as problematic. But are we so naïve to think that only the most problematic facets of a phenomenon play a role in that phenomenon? Researchers have known for a long time that many causally important aspects of mental disorders are “ego-syntonic” (that is, they are not immediately distressing to the patient). For instance, a patient suffering from OCD is likely to report uncomfortable obsessions and compulsions as potential problems to fix, but may not realize that his or her cognitive style of intolerance of uncertainty is contributing to the problem. This focus on only the visibly distressing aspects of a disorder (similar to a medical check-up) seems to make intuitive sense for client whose distress brought them into therapy in the first place, but may not provide a complete picture of the true causal structure of the problem.
When imagining a causal system of a mental disorder, we can also hypothesize that there may be some protective factors involved. These potential “brakes” in the system will obviously be missed by symptom manuals, which focus only on the negatives.
3) Symptoms are not supposed to interact with each other
Ironically, many symptom manuals were designed in direct opposition to the network view. That is, those designing the measures intentionally tried to pick symptoms which did not interact with one another, for psychometric reasons. For instance, clinicians are often trained in diagnostic interviews to attempt to separate “simple tiredness from sleep issues” from “a different, more profound tiredness associated with depression”, and only count the latter as a symptom. This is obviously problematic if we are attempting to put symptoms into a network, which focuses on the relatedness of symptoms to one another in the emergence of a disorder.
In addition, some manualized symptoms really do seem to be reflective of problems, rather than causally important. For instance, “weight loss” is often included as a symptom of depression. It is easy to see how weight loss could be reflective of other depression symptoms. However, it is somewhat difficult to imagine that weight loss is responsible for causing depression (at least in a majority of people). If networks are supposedly causal systems, it doesn’t make much sense to include this particular symptom.
The expanded network approach
Recently, our lab published a commentary on Borsboom’s review, proposing an expanded view which may help with some of these problems. Instead of relying wholly on symptoms from diagnostic manuals, we propose that networks should include variables that are plausible causal candidates in the etiology or maintenance of mental disorders. This still includes symptoms, but also includes other variables such as cognitive factors, biological factors, and protective factors.
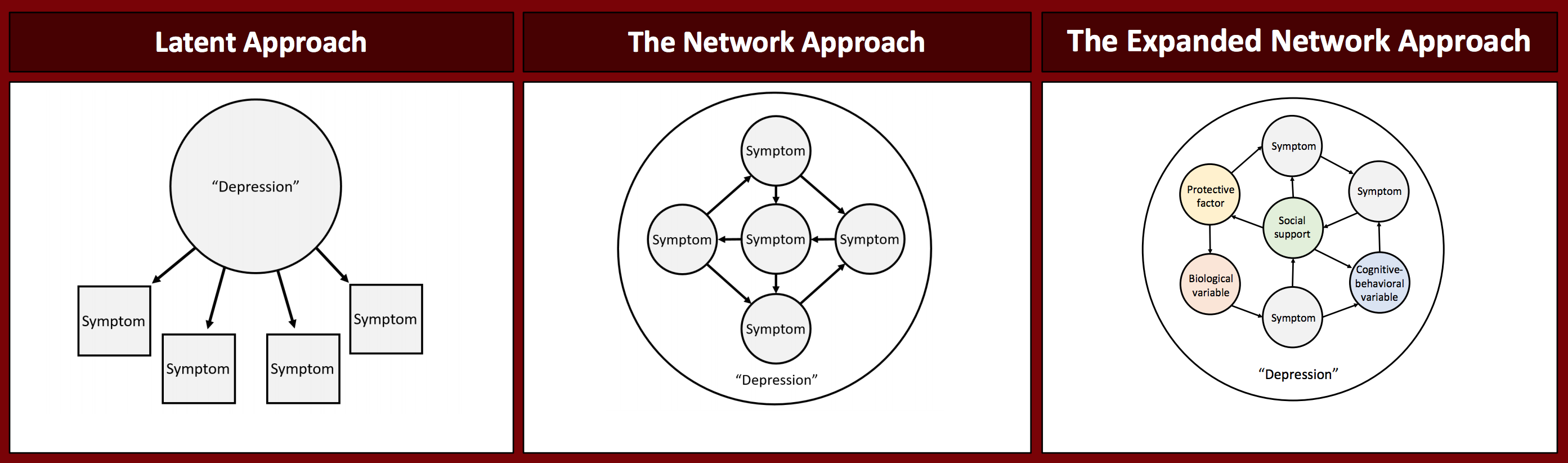
We aren’t the only ones who have thought along these lines. In Eiko Fried and Angelique Cramer‘s recent comprehensive summary of challenges to the network approach, they discuss problems with the term “symptom” and how focusing primarily on symptoms has led network researchers to ignore important elements of mental disorders. Related, the paper includes a discussion on how more static components that play a role in mental disorders (e.g., an initial trauma that sparked PTSD or personality traits) might be conceptualized from a dynamic systems point of view.
By focusing network analyses only on symptoms, what have we missed? Between the commentary and the review, here are some suggested possibilities: impairment of functioning, information processing biases, maladaptive (or adaptive) schemas, metacognitive beliefs, life events, self-esteem, social interactions, rejection events, physical activities, and substance abuse.
In the meantime, some researchers have already been putting the rubber to the road by including non-symptom nodes in network analyses. Here are some prime examples of nodes in recent empirical publications that follow the expanded network approach:
- Attentional control as a node in social anxiety disorder
- Resilience as a protective node in depression
- Access to food as a node in trauma-related problems among war survivors
- Childhood sexual abuse as a node in psychotic disorders
- Impairment of mental and physical functioning in PTSD networks of trauma-exposed veterans
Are symptoms sufficient for network analyses going forward? Or are other causal candidates also important to include as nodes? The future is up to you!
Written by: Payton Jones (payton_jones@g.harvard.edu) and Haley Elliott (haleyelliott@college.harvard.edu)
Great blog Payton & Haley! Here my thoughts.
1) Historically, Angelique Cramer’s (et al.) 2010 comorbidity paper uses symptoms because they are a good starting point for problems people have. And the idea of network theory is that “problems attract problems”. So I think symptoms are a convenient starting point for which ample data is available, and I don’t believe anybody would argue that we should solely focus on symptoms (including Denny who in my reading uses symptoms synonymously with problems in his World Psychiatry paper). And I think the discussion “why have many papers modeled symptoms” is a bit similar to the very fruitful discussion Angelique and I had with a reviewer for our challenges paper. The reviewer pointed out that most prior network papers have modeled “depression”, “PTSD”, “generalized anxiety disorder” etc., and that this is weird given the high comorbidity rates among disorders, and given the criticism of some network papers about the validity of these disease categories. Angelique and I wholeheartedly agreed, and believe the reason why papers often focused on DSM symptoms is similar to the reason papers often focused on DSM disorders: it’s probably the best way to start (cf. p.6 of the paper).
2) You are right that many researchers have focused on symptoms — mostly symptoms as defined in the DSM — and that it would be a good idea to look into other problems as well. My thoughts on the topic were, as you mention in the blog, recently published in the challenges paper I co-wrote with Angelique. First, in order to answer what items are relevant to a dynamic system, we aim to define dynamic system. We then move on to discuss that there are variables within the system, and variables outside of the system (in the “external field”), that can influence the system. And then discuss that things are probably not so easy, and depending on the time-scale you measure your variables, and your definition of the system, some variables meet criteria for both within the system and being part of the external field. You mention a bunch of examples of variables in the blog post, and the challenge now is to think about how to include them into models (gender just doesn’t really evolve on the same time scale than irritability, and splitting groups on covariates is not always feasible or sufficiently informative for dynamical systems).
3) Many researchers and clinicians have argued that that symptoms are definitely not the only way to look at this. Marieke Wichers comes to mind, who stated in a great overview paper in 2013 that micro-level patterns of experience and behavior contribute to our understanding of macro-level symptoms and disorders.
Thanks for your insights, Eiko! Glad to see some addition to the discussion. I have some additional thoughts about what you’ve mentioned:
I like the idea of “problems attract problems”, but does this leave room for protective factors like resilience ? What about variables that aren’t necessarily “problems”, but are important in certain psychopathology, like attention processing?
Denny does use the exact phrase “symptoms from diagnostic manuals” in his World Psychiatry paper, but perhaps this was at the nudge of a reviewer. After all, he gave favorable reviews for this very commentary (reviewers are public on Frontiers), and was also a co-author on at least one recent paper using non-symptom nodes.
As I’ve talked to other network researchers, I have definitely received the impression that most people are really interested in networks that represent the mechanisms of etiology and maintenance of psychopathology, and symptoms are merely a piece of that. I agree that this has been hinted at in many prior publications. This commentary was merely an attempt to formalize this viewpoint.
Full agreement! I just wanted to provide a bit of historical context and give you my own opinion on why many network papers so far have focused on specific disorders — and within these papers — often on symptoms: I think it’s a reasonable starting point, and I’m happy to see so many recent papers move beyond that.
Pingback: A summary of my academic year 2017 – Eiko Fried